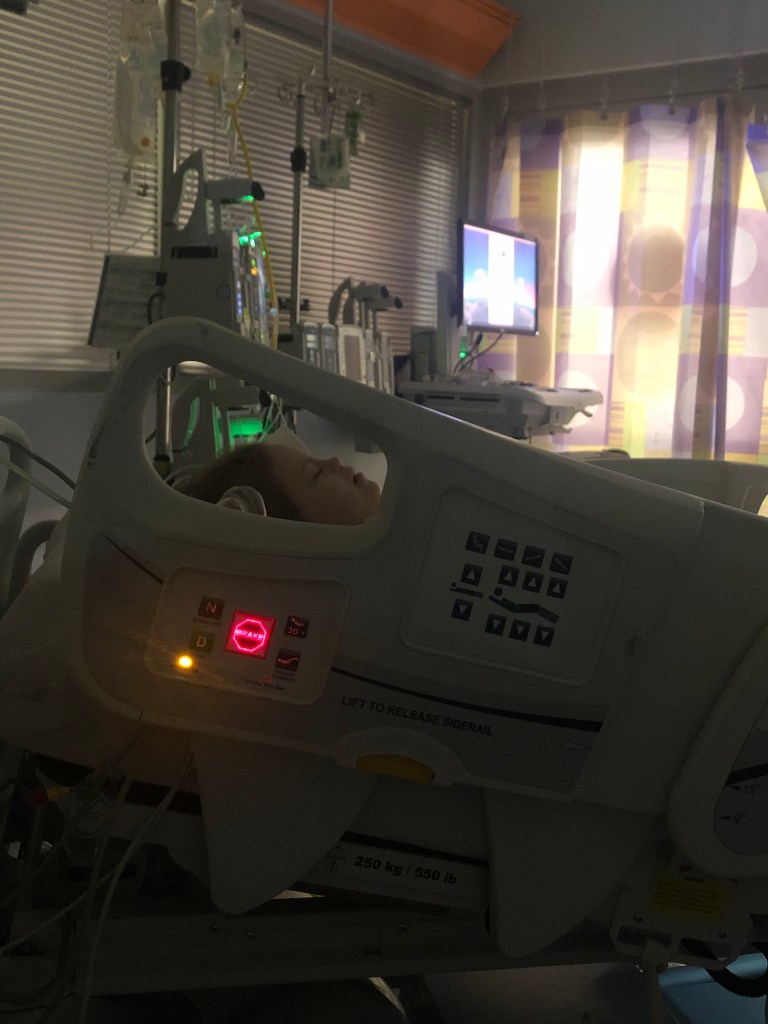
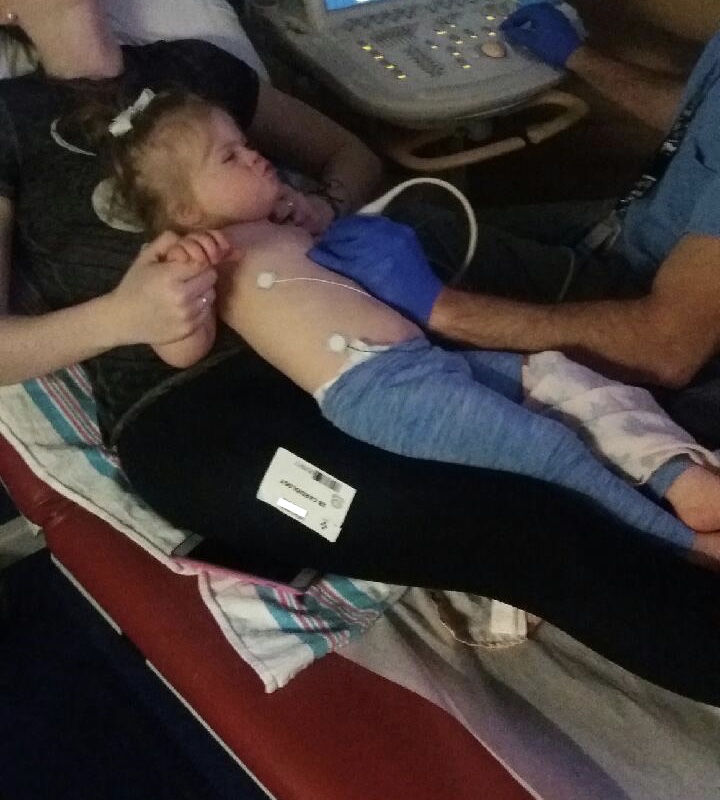
A year ago I was falling apart, losing the years worth of strength I’d built up as a special needs mom. The armor dissolving. The walls crumbling. The tightly wound thread of control unraveling. It started on a Friday morning in August and worsened with each passing month, counting down to January 3.
September 3 – This isn’t fair.
October 3 – I can’t believe we have to do this.
November 3 – This better be worth it.
December 3 – I’m not going to make it.
When December hit I was no longer counting down weeks or days. Time was marked by each breath I forced into my lungs. I desperately tried to stay busy, preoccupy myself with work and terrible Netflix shows, but my mind and body couldn’t fight the anxiety. I lost sleep, gained a stress rash, and spent weeks on the verge of a panic attack. In hindsight I’m not sure what I could have done differently because nothing would have made me feel better about Hannah having another heart surgery.
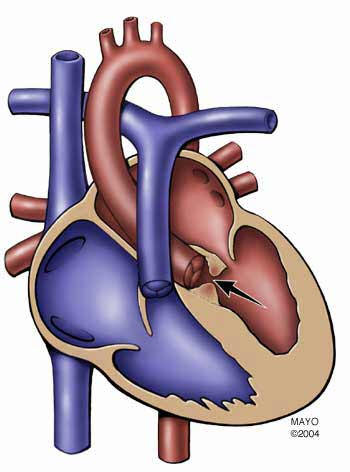
Hannah’s first heart surgery made sense. She was sick. Her life was measured in ounces and milliliters. As terrifying as the experience was, we were in survival mode. Life was a new parent / new diagnosis haze, checking off each weigh in, each echo, each day that brought us closer to Hannah having a healthy heart. We tamped down our fear knowing Hannah would never remember any of it.
The second heart surgery did not make sense, even though we had known for years it needed to happen at some point. As each visit to cardiology passed without hitting that “some point” we created a fairytale that the day would never arrive. And then it did. Hannah was healthy. She was finally back in school with her friends after a year of remote learning. Worst of all, she was old enough to remember. The guilt and betrayal we felt knowing our girl, who is afraid of having a bandaid pulled off her skin, was about to live her hardest weeks was unbearable.
It’s hard to believe it’s only been one year since the surgery. We achieved our goal to pack the rest of 2022 with so much joy and fun that Hannah wouldn’t remember missing 8 weeks of school. Maybe it was a little bit for us too. December came and went, and I tried to convince myself it was safe to reflect on the experience but each time I was met with tears and a familiar tightness in my chest. Now, with a quiet house and some cupcake-fueled courage, I can finally close this chapter.