The morning after Hannah’s birth Pete visited me in the hospital, then headed to the children’s hospital with his mom to see Hannah. His mom had called the hospital to ask about me visiting while I had the flu and she was told I could not and that my breast milk could not be used due to the Tamiflu I was taking. Luckily, the doctor they met assured them that I could absolutely be there as long as I wore a gown, mask, and gloves and that my milk would be safe for Hannah. My parents came to my hospital and stayed with me until I was discharged that afternoon.
Pete returned home to give us an update on Hannah. He was restless and had a hard time being home knowing Hannah was alone in the hospital. We did a lot of crying that night.
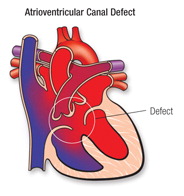
The next day, Pete’s parents, my parents, Pete and I all headed up to the hospital to see Hannah in the PICU. The on-call doctor explained the heart defect to us. Hannah had an AV Canal defect: a hole in the middle of her heart that was allowing oxygen-rich blood and oxygen-poor blood to mix. Her little body wasn’t getting enough oxygen and her lungs were overloaded from the extra oxygen in the blood.
I held Hannah for a while in the ICU and then she was transferred up to a regular floor. The next few days were a blur of nurses and specialists. When the nurses weren’t taking vitals, then a lactation consultant was helping me nurse Hannah, or a speech therapist watched Hannah’s suck/swallow/breathe rhythm, or another hearing test was being done. One person would leave and another would enter. My parents took turns staying with me at the hospital while Pete was at work. They would make sure I ate actual meals and asked the doctors questions that I didn’t think of. Pete would drive up every afternoon after work and we’d leave when Hannah fell asleep. I wish I would have been strong enough to stay at the hospital with her but it was too much with the flu and postpartum discomfort.
A cardiologist visited every day with updates on Hannah’s status and to answer any questions we may have thought of overnight. She was incredibly kind and thorough, never rushing out of the room. She assured us that even if Hannah’s heart defect had been diagnosed prenatally it wouldn’t have been considered a high risk pregnancy. Nothing would have changed except learning some new vocabulary. We would have had the same labor and the same delivery. Hannah still would have been transferred to the children’s hospital that evening but with less uncertainty.
The other main concern during the week was Hannah’s weight gain. We were fortunate that she was born chubby at 8 pounds 8 ounces and never lost any weight like most newborns do (I blame that on the extra fluid her body was holding on to). The nurses were quite rigid about feeding Hannah every three hours on the dot. Breastfeeding was difficult. I’d have to warn the nurses I was taking Hannah off her monitors, strip her down, weigh her, try to feed her without her falling asleep, weigh her again, dress her, and finally hook her back up to the monitors. Hannah performed well in front of the lactation consultants but I struggled on my own without the extra two hands. If Hannah’s weight didn’t increase enough after each meal I felt like a failure.
One night as Pete and I were leaving, the nurse warned us that Hannah would need an NG tube if she didn’t eat well overnight. Imagine my surprise when I arrived the next morning to see a little yellow tube taped to her cheek and disappearing into her nose. The nurse had inserted it during the night and it was the kick in the butt that Hannah needed to finish a bottle. She was never even fed through the tube so it was removed after about 12 hours. The cardiologist finally told the nurses to relax with the calorie counting because Hannah was stable and going home soon.
Hannah needed two final tests before being discharged. She didn’t pass her first hearing test, possibly because of the NG tube affecting her inner ear balance, so another test was administered. with the same results – no reaction to the lowest decibels. The audiologist explained that it’s common with newborn because they’d been living in fluid for 9 months and that the test would need to be repeated a few weeks later.
The second test was to ensure Hannah’s oxygen levels didn’t drop in the car seat. The nurse strapped Hannah in, still connected to the monitor, and we let her sleep. It was supposed to be an hour long test but the cardiologist stopped it after about ten minutes because Hannah’s oxygen levels never dipped.
The remainder of the afternoon was a waiting game. Hannah was taken off the monitors, which meant I could hold her whenever I wanted. The cardiologist stopped by one last time to make sure we were fully educated on the heart defect. We signed a lot of papers. We bundled Hannah up in an outfit it took me months to find. We got stuck in traffic and heard her cry for the second time in her life. Six days after she was born, we welcomed our little girl home.